Why States Are Adopting MLTSS
Managed Long Term Services and Supports (MLTSS) refers to the delivery of long term services and supports through capitated Medicaid managed programs. Increasing numbers of states are using MLTSS as a strategy for expanding home and community-based services, promoting community inclusion, ensuring quality, and increasing efficiency.
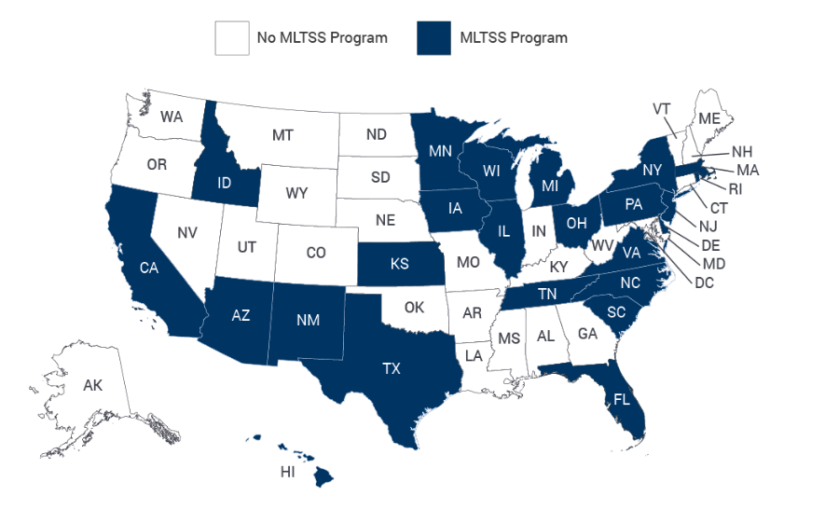
According to NASUAD, as of June of last year, 24 states operate managed long-term services and supports (MLTSS) programs, in which state Medicaid agencies contract with managed support plans to deliver long-term services and supports.
Please refer to the state-wide adoption map above. It’s important to look at why states are moving toward MLTSS to understand it’s value. Here are four fundamental realities driving this change.
-
With MLTSS, accountability rests with a single entity
In a more comprehensive accountability environment of MLTSS, it’s easier to measure the extent to which the system operates efficiently, ethically, transparently and effectively in achieving desired outcomes. Data is more consistent. Communication is more secure. And strategic and administrative directions are set and pursued under one roof.
Delivery of services is not fragmented among several organizations but coordinated and more efficiently provided, with full communication among staff, administration, and executive functions, especially if it is facilitated by a networked, secure software system such as iCareManager.
This means cost savings, better support, more transparency, and better outcomes.
-
Budget predictability
Decades of failed efforts to constrain health care costs have made both states and providers acutely aware of the overall state budget tradeoffs, risks, and shortfalls of inadequate models around which to create and execute budgets.
From a provider point of view, episode-based funding is highly unpredictable and leads to fluctuating income, fluctuating capabilities based on the ups and downs of income, and fluctuating quality of services. Effective planning is also extremely adversely affected.
MLTSS, on the other hand, allows known and predictable capitation payments. A PMPM (per member, per month) funding structure provides stability in income which allows more efficient, informed, strategic planning.
-
Bending the cost curve
Furthermore, health care costs keep climbing on a steep curve. MLTSS bends that curve downward, providing states with more stable, more predictable costs. This, in turn, allows states to identify or create stable sources of revenue to supply these funds. The fluctuations in needed levels of actual services to a given population of individuals evens out to a trend line discoverable in data. States and service providers, using data stored and retrievable in a system such as iCareManager, can more efficiently plan, bending the cost curve down over time while providing services more efficiently
-
Rebalancing the system
A capitation payments model in MLTSS reduces variation in funding and allows providers to maximize the benefits of organizational expenditures.
It also helps ensure people are treated in the right setting of support, with the right clinical or support workforce, and with the right tools and resources.
A more balanced system in this way enables more efficiency in managing supply and resource chains. All of these benefits, together with data, allows executives to set strategic direction effectively.
States will continue to adjust, innovate and adopt MLTSS. Data and speed of communication are key components of the realities driving and enabling this change. The ability to see in the data what’s coming, and to see also stability in funding and budgets, will help to bend costs downward and to improve results for individuals, providers, and states.